Insights
Insights – Spot Trends, Improve Payer Outcomes



Overview
Data-Driven Decision Making for Better Outcomes
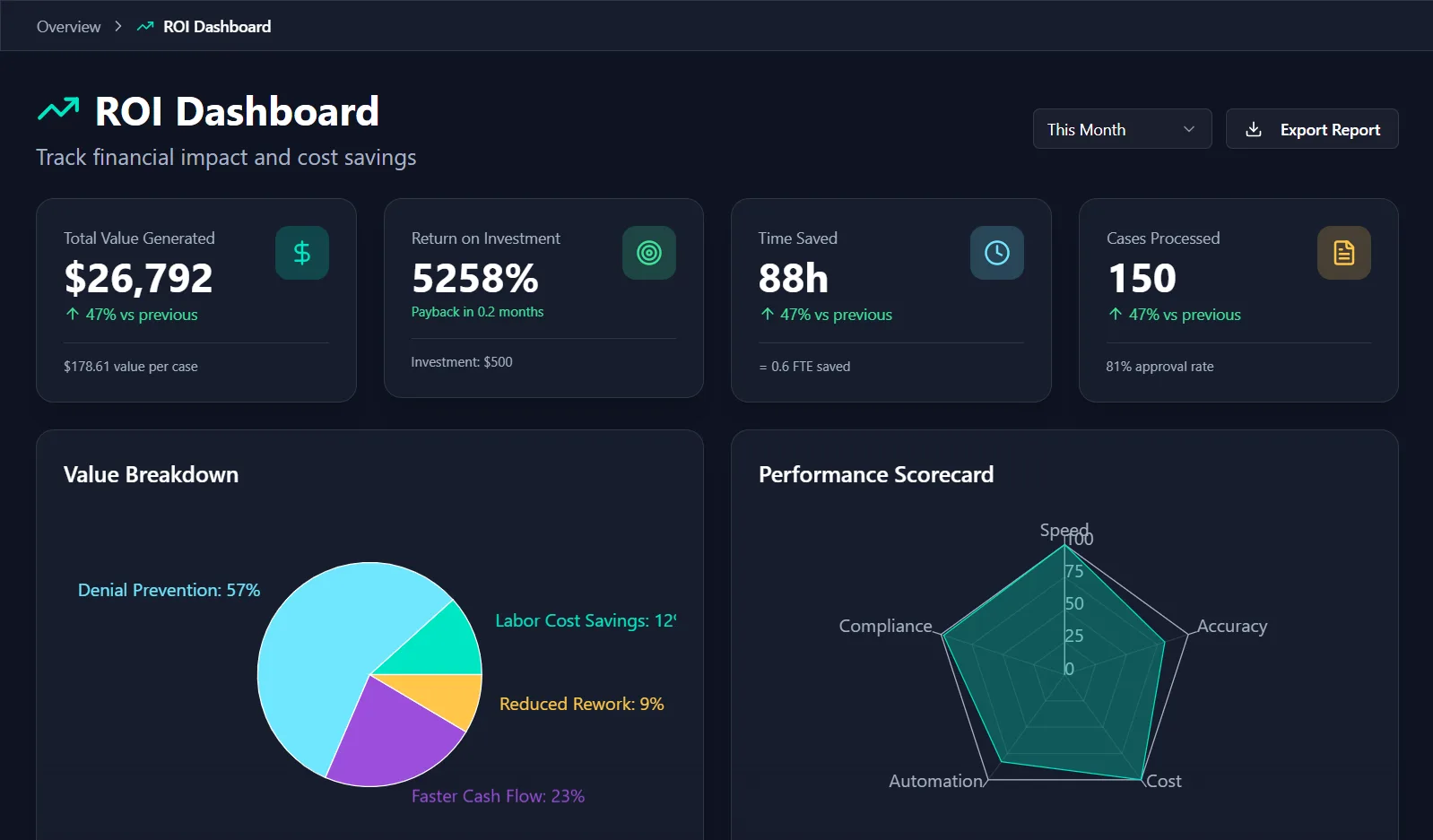
Every authorization generates valuable data—approval rates, processing times, denial reasons, payer behaviors, and more. But without the right tools, this data sits unused while opportunities for improvement go unnoticed. SuperAuth.ai’s Insights platform transforms raw authorization data into powerful intelligence that drives better outcomes.
Our analytics engine analyzes thousands of data points across all your authorizations, identifying patterns invisible to human observation. Discover which payers approve fastest, which documentation increases approval likelihood, which procedures face the most denials, and which staff members achieve the best outcomes.
KEY BENEFITS
Identify Denial Patterns
AI analyzes thousands of denials to identify common patterns, root causes, and prevention strategies—reducing future denials by up to 40%.
Optimize Payer Relationships
See which payers approve fastest, have highest success rates, and best documentation requirements—enabling data-driven payer negotiations.
Predict Approval Likelihood
Machine learning predicts which authorizations will be approved or denied before submission, allowing proactive intervention.
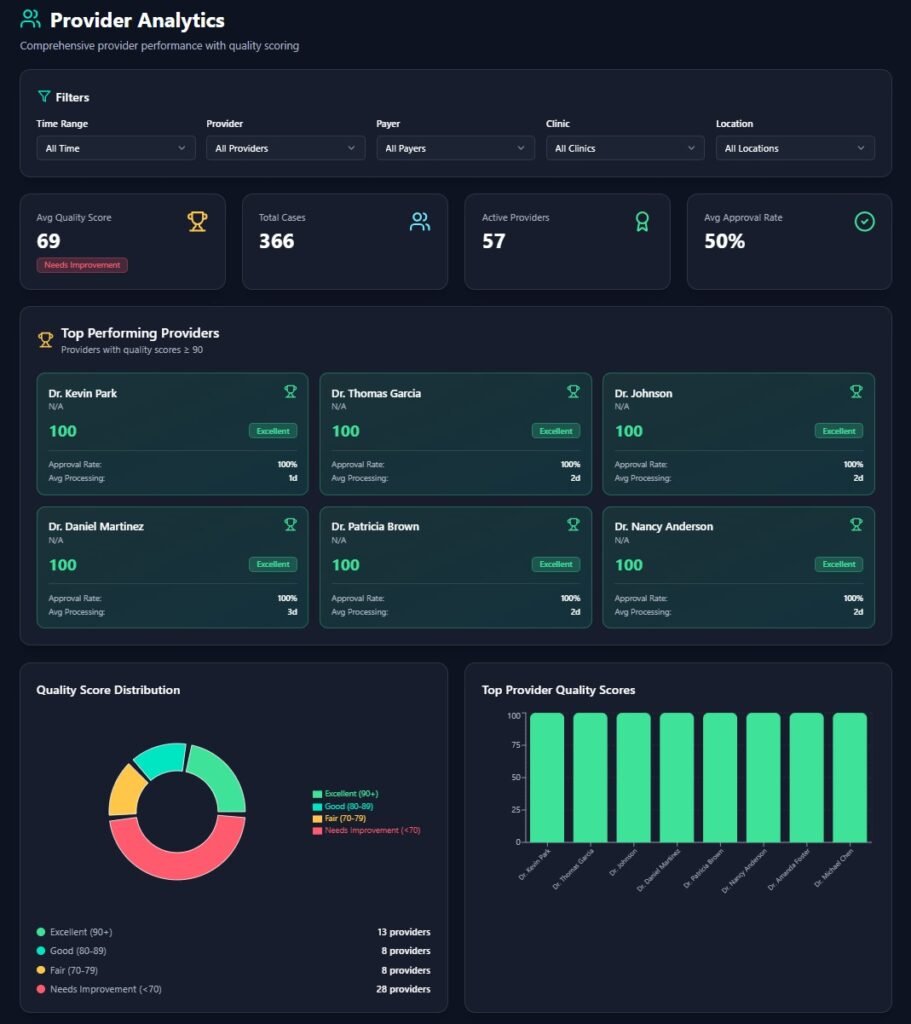
Track Team Performance
Monitor individual and team metrics including processing speed, approval rates, and quality scores to drive continuous improvement.

HOW IT WORKS
From Data to Actionable Insights in 5 Steps
AI continuously captures data from every authorization—submission details, payer responses, processing times, outcomes, and user actions.
Step 2: Intelligent AnalysisAdvanced algorithms analyze patterns across thousands of authorizations, identifying trends, anomalies, and opportunities for improvement.
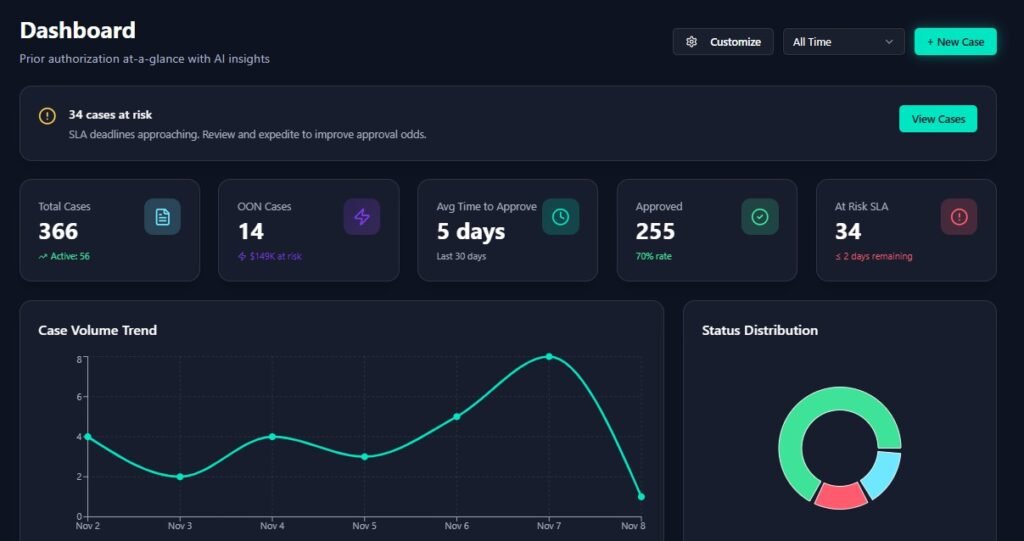
Step 3: Visual DashboardsComplex data is transformed into intuitive visualizations—charts, graphs, heat maps, and scorecards that make insights immediately clear.
Step 4: Actionable RecommendationsAI provides specific recommendations: which documentation to improve, which payers to prioritize, which processes to optimize.
Step 5: Continuous LearningThe system learns from every authorization, continuously refining predictions and recommendations to improve accuracy over time.
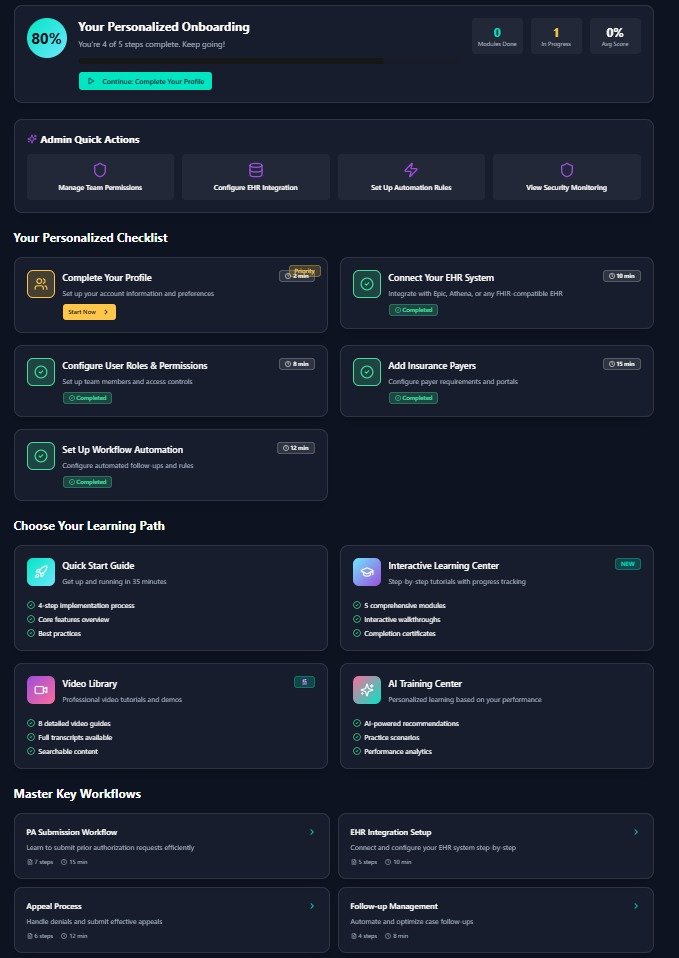

Executive Dashboard
High-level KPIs and trends including overall approval rates, authorization volume trends, revenue impact, team productivity, and month-over-month comparisons.
Manager Dashboard
Operational metrics for workflow optimization—team performance, queue status and backlogs, processing time trends, error rates, and resource allocation.
Clinical Dashboard
Provider-focused metrics including personal approval rates, pending authorizations, urgent cases requiring attention, documentation quality scores, and peer comparisons.
Payer Relations Dashboard
Relationship management insights—payer-specific performance, communication history, contract compliance, negotiation leverage points, and relationship health scores.
ADVANCED ANALYTICS FEATURES
Trend Analysis
Visualize trends over time with interactive charts showing approval rate trends, volume patterns, seasonal variations, and long-term improvements.
Cohort Analysis
Compare different groups including authorization types, patient populations, payers, procedures, staff members, and time periods.
Root Cause Analysis
Drill down to understand why denials happen—common denial reasons, documentation issues, timing problems, and payer-specific requirements.
Benchmarking
Compare your performance against industry standards, specialty-specific norms, historical baselines, and peer organizations.
Custom Reports
Build custom reports with drag-and-drop—select metrics and dimensions, apply filters, choose visualization types, and schedule automatic delivery.
Alert System
Set up intelligent alerts for approval rates dropping below threshold, unusual denial patterns, processing time increases, and volume spikes.

HOW IT WORKS
From Data to Actionable Insights in 5 Steps
AI continuously captures data from every authorization—submission details, payer responses, processing times, outcomes, and user actions.
Step 2: Intelligent AnalysisAdvanced algorithms analyze patterns across thousands of authorizations, identifying trends, anomalies, and opportunities for improvement.
Step 3: Visual DashboardsComplex data is transformed into intuitive visualizations—charts, graphs, heat maps, and scorecards that make insights immediately clear.
Step 4: Actionable RecommendationsAI provides specific recommendations: which documentation to improve, which payers to prioritize, which processes to optimize.
Step 5: Continuous LearningThe system learns from every authorization, continuously refining predictions and recommendations to improve accuracy over time.
Have Any Questions?
Find answers to commonly asked questions about SuperAuth.ai’s platform, features, and implementation process.
Can we export data for presentation to leadership?
Yes. Export charts, graphs, and reports in PDF, PowerPoint, or image formats ready for executive presentations.
How far back does historical data go?
We retain all historical analytics data for the lifetime of your account, allowing long-term trend analysis.
Can we compare our performance against other organizations?
Yes. Enterprise customers can access anonymized benchmark data from similar organizations in their specialty and region.
Are insights available in real-time or delayed?
Real-time. Dashboards update immediately as new authorization data is processed, giving you current visibility.

Transforming prior authorization with AI-powered automation. Get approvals faster, reduce administrative burden, and improve patient care.